Blood Donor
Blood Group: A (Positive)
Membership No.: 1
Present Address: Nizkunjara, Chagolniya, Feni
Permanent Address: Village # Nizkunjara, Union # Gopal, Upazila # Chhagalniya, District # Feni, Division # Chattogram
Date of Birth: 01-01-1970
Place of Birth.: Feni

Phone: 01674849616
E-mail Address: nkalambhuiyan@gmail.com
Social Media Address:
Blood Group: A (Positive)
Religion: Islam
Gender: Male
Blood Group: A (Negative)
Blood Group: B (Positive)
Blood Group: B (Negative)
Blood Group: AB (Positive)
Blood Group: AB (Negative)
Blood Group: O (Positive)
Blood Group: O (Negative)
Blood Type Information
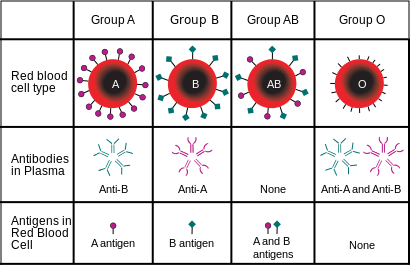
A blood type (also called a blood group) is a classification of blood based on the presence or absence of inherited antigenic substances on the surface of red blood cells (RBCs). These antigens may be proteins, carbohydrates, glycoproteins, or glycolipids, depending on the blood group system. Some of these antigens are also present on the surface of other types of cells of various tissues. Several of these red blood cell surface antigens can stem from one allele (or very closely linked genes) and collectively form a blood group system. Blood types are inherited and represent contributions from both parents. A total of 32 human blood group systems are now recognized by the International Society of Blood Transfusion (ISBT) The two most important ones areABO and the RhD antigen; they determine someone's blood type (A, B, AB and O, with + and − denoting RhD status). Many pregnant women carry a fetus with a blood type which is different from their own, and the mother can form antibodies against fetal RBCs. Sometimes these maternal antibodies areIgG, a small immunoglobulin, which can cross the placenta and cause hemolysis of fetal RBCs, which in turn can lead to hemolytic disease of the newborn called erythroblastosis fetalis, an illness of low fetal blood counts that ranges from mild to severe. Sometimes this is lethal for the fetus; in these cases it is called hydrops fetalis.
ABO blood group system
The ABO system is the most important blood-group system in human-blood transfusion. The associated anti-A and anti-B antibodies are usually immunoglobulin M, abbreviated IgM, antibodies. ABO IgM antibodies are produced in the first years of life by sensitization to environmental substances such as food, bacteria, and viruses. The O in ABO is often called 0 (zero, or null) in other languages.
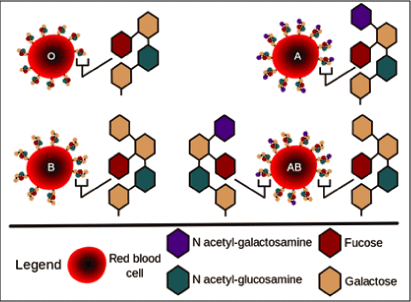
ABO blood group system: diagram showing the carbohydrate chains that determine the ABO blood group
Rh blood group system
The Rh system (Rh meaning Rhesus) is the second most significant blood-group system in human-blood transfusion with currently 50 antigens. The most significant Rh antigen is the D antigen, because it is the most likely to provoke an immune system response of the five main Rh antigens. It is common for D-negative individuals not to have any anti-D IgG or IgM antibodies, because anti-D antibodies are not usually produced by sensitization against environmental substances. However, D-negative individuals can produce IgG anti-D antibodies following a sensitizing event: possibly a fetomaternal transfusion of blood from a fetus in pregnancy or occasionally a blood transfusion with D positive RBCs. Rh disease can develop in these cases. Rh negative blood types are much less common in proportion of Asian populations (0.3%) than they are in White (15%). The presence or absence of the Rh antigens is signified by the + or − sign, so that for example the A− group does not have any of the Rh antigens.
Other blood group systems
32 blood-group systems have been identified, including the ABO and Rh systems.Thus, in addition to the ABO antigens and Rh antigens, many other antigens are expressed on the RBC surface membrane. For example, an individual can be AB, D positive, and at the same time M and N positive (MNS system), K positive (Kell system), Lea or Leb negative (Lewis system), and so on, being positive or negative for each blood group system antigen. Many of the blood group systems were named after the patients in whom the corresponding antibodies were initially encountered.
Red blood cell compatibility
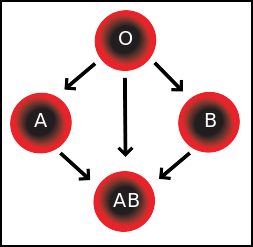
Blood group AB individuals have both A and B antigens on the surface of their RBCs, and their blood plasma does not contain any antibodies against either A or B antigen. Therefore, an individual with type AB blood can receive blood from any group (with AB being preferable), but cannot donate blood to any group other than AB. They are known as universal recipients.
Blood group A individuals have the A antigen on the surface of their RBCs, and blood serum containing IgM antibodies against the B antigen. Therefore, a group A individual can receive blood only from individuals of groups A or O (with A being preferable), and can donate blood to individuals with type A or AB.
Blood group B individuals have the B antigen on the surface of their RBCs, and blood serum containing IgM antibodies against the A antigen. Therefore, a group B individual can receive blood only from individuals of groups B or O (with B being preferable), and can donate blood to individuals with type B or AB.
Blood group O (or blood group zero in some countries) individuals do not have either A or B antigens on the surface of their RBCs, and their blood serum contains IgM anti-A and anti-B antibodies against the A and B blood group antigens. Therefore, a group O individual can receive blood only from a group O individual, but can donate blood to individuals of any ABO blood group (i.e., A, B, O or AB). If a patient in a hospital situation were to need a blood transfusion in an emergency, and if the time taken to process the recipient's blood would cause a detrimental delay, O Negative blood can be issued. They are known as universal donors.
Red blood cell compatibility table
| Recipient | Donor | |||||||
|---|---|---|---|---|---|---|---|---|
| O− | O+ | A− | A+ | B− | B+ | AB− | AB+ | |
| O− | ||||||||
| O+ | ||||||||
| A− | ||||||||
| A+ | ||||||||
| B− | ||||||||
| B+ | ||||||||
| AB− | ||||||||
| AB+ | ||||||||
Table note 1. Assumes absence of atypical antibodies that would cause an incompatibility between donor and recipient blood, as is usual for blood selected by cross matching. An Rh D-negative patient who does not have any anti-D antibodies (never being previously sensitized to D-positive RBCs) can receive a transfusion of D-positive blood once, but this would cause sensitization to the D antigen, and a female patient would become at risk for hemolytic disease of the newborn. If a D-negative patient has developed anti-D antibodies, a subsequent exposure to D-positive blood would lead to a potentially dangerous transfusion reaction. Rh D-positive blood should never be given to D-negative women of child bearing age or to patients with D antibodies, so blood banks must conserve Rh-negative blood for these patients. In extreme circumstances, such as for a major bleed when stocks of D-negative blood units are very low at the blood bank, D-positive blood might be given to D-negative females above child-bearing age or to Rh-negative males, providing that they did not have anti-D antibodies, to conserve D-negative blood stock in the blood bank. The converse is not true; Rh D-positive patients do not react to D negative blood. This same matching is done for other antigens of the Rh system as C, c, E and e and for other blood group systems with a known risk for immunization such as the Kell system in particular for females of child-bearing age or patients with known need for many transfusions.
Plasma compatibility
Recipients can receive plasma of the same blood group, but otherwise the donor-recipient compatibility for blood plasma is the converse of that of RBCs: plasma extracted from type AB blood can be transfused to individuals of any blood group; individuals of blood group O can receive plasma from any blood group; and type O plasma can be used only by type O recipients.
Plasma compatibility table
| Recipient | Donor | |||
|---|---|---|---|---|
| O | A | B | AB | |
| O | ||||
| A | ||||
| B | ||||
| AB | ||||
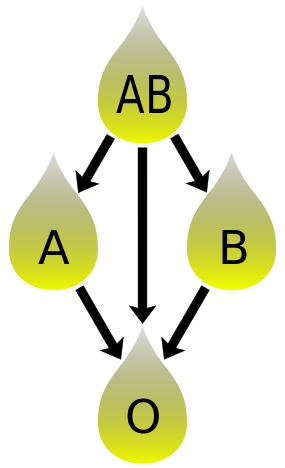
Table note 1. Assumes absence of strong atypical antibodies in donor plasma Rh D antibodies are uncommon, so generally neither D negative nor D positive blood contain anti-D antibodies. If a potential donor is found to have anti-D antibodies or any strong atypical blood group antibody by antibody screening in the blood bank, they would not be accepted as a donor (or in some blood banks the blood would be drawn but the product would need to be appropriately labeled); therefore, donor blood plasma issued by a blood bank can be selected to be free of D antibodies and free of other atypical antibodies, and such donor plasma issued from a blood bank would be suitable for a recipient who may be D positive or D negative, as long as blood plasma and the recipient are ABO compatible.
Blood Types and the Population
| Blood Group | Caucasians | African American | Hispanic | Asian |
|---|---|---|---|---|
|
O +
|
37%
|
47%
|
53%
|
39%
|
|
O -
|
8%
|
4%
|
4%
|
1%
|
|
A +
|
33%
|
24%
|
29%
|
27%
|
|
A -
|
7%
|
2%
|
2%
|
0.5%
|
|
B +
|
9%
|
18%
|
9%
|
25%
|
|
B -
|
2%
|
1%
|
1%
|
0.4%
|
|
AB +
|
3%
|
4%
|
2%
|
7%
|
|
AB -
|
1%
|
0.3%
|
0.2%
|
0.1%
|
Some patients require a closer blood match than that provided by the ABO positive/negative blood typing. For example, sometimes if the donor and recipient are from the same ethnic background the chance of a reaction can be reduced. That’s why an African-American blood donation may be the best hope for the needs of patients with sickle cell disease, 98 percent of whom are of African-American descent.
Blood Types and the Population
It’s inherited. Like eye color, blood type is passed genetically from your parents. Whether your blood group is type A, B, AB or O is based on the blood types of your mother and father.
This chart shows the potential blood types you may inherit.
| Parent 1 Blood Type | Parent 2 Blood Type | Child's Possible Blood Types | Child's Impossible Blood Types |
|---|---|---|---|
| O | O | O | A, B, AB |
| O | A | A, O | B, AB |
| O | B | B, O | A, AB |
| O | AB | A, B | O, AB |
| A | A | A, O | B, AB |
| A | B | A, B, AB, O | None |
| A | AB | A, B, AB | O |
| B | B | B, O | A, AB |
| B | AB | A, B, AB | O |
| AB | AB | A, B, AB | O |
Note: If you have questions about paternity testing or about blood group inheritance, your primary care physician should be able to provide you with an appropriate referral. Testing difficulties can cause exceptions to the above patterns. ABO blood typing is not sufficient to prove or disprove paternity or maternity.